Case of the month: The sad story of Pancreatitis !
A 30-year-old male patient was admitted to our hospital with a history of epigastric pain radiating to the back of 4 days’ duration. The pain was associated with recurrent vomiting on the first day. The patient had been a chronic alcoholic for the past 4 years.
There was no history of jaundice, abdominal distension. There was no history of previous abdominal pain or diabetes mellitus.
On examination:
The patient was stable hemodynamically; he had epigastric tenderness and no organomegaly no free fluid in the abdominal cavity.Rest of clinical exam was normal.
Investigations :
The investigation revealed a hemoglobin of 11 gm/dL total leukocyte count of 17,300/mm and serum amylase of 400 IU/mL (up to 100 IU/mL), and results of serum biochemistry and chest radiograph were normal.
A contrast-enhanced CT (CECT) revealed an edematous pancreas with multiple areas of necrosis in the head and tail regions. There was peripancreatic fluid collection extending to left pararenal space. Vascular structures were normal.
Hospital course :
The patient was managed with IV fluids , Ryles tube aspiration .
A week after admission, he developed a high-grade fever. Correspondingly, he had leukocytosis (19,000/mm3 ), but his blood and urine cultures were sterile. Abdominal US showed a fluid collection with internal echoes in the left iliac fossa, and an 8F pigtail catheter was placed in the collection. Purulent material was drained, but its culture was sterile.The patient was started on injection Meropenum
Three days later he developed 3 bouts of melaena, with a drop in hemoglobin to 7.0 gm/dL.He was resuscitated and a second CECT was performed, which revealed a bulky pancreas with multiple hypodense areas of necrosis and marked peripancreatic inflammation extending onto the posterior wall of the stomach, greater omentum, gastrocolic and gastrosplenic ligaments, root of mesentery, and left paracolic gutter (Fig.1).
 |
| Fig 1 CT scan abdomen showing severe pancreatitis |
There was an eccentric thrombus in the superior mesenteric vein at its junction with the splenic vein, but the splenoportal axis was patent. The patient then underwent endoscopy, which revealed a normal esophagus, and a large clot was seen along the lesser curvature of the stomach. Multiple fistulous tracts were seen on the posterior wall of the stomach leading into the peritoneal cavity (Fig. 2).
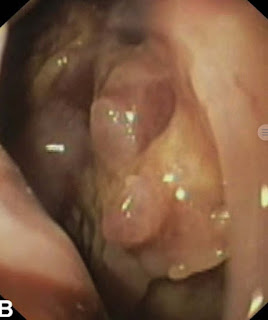 |
| Fig 2 EGD showing peritoneal cavity pancreato gastric fistula |
The endoscope could be passed into the duodenum, and no other source of bleeding could be ascertained. A diagnosis of pancreatico gastric fistula was made, and laparotomy was performed. Operative findings revealed that the entire omentum was inflamed and studded with fat necrosis. Necrotic material eroded the whole of the greater curvature and posterior wall of the stomach. The splenic hilum was actively bleeding. All of the necrotic tissue was removed after opening the gastrocolic ligament. A splenectomy was performed after ligation of the splenic pedicle, the stomach was repaired, and a gastrotomy was performed using a 24F mallecot catheter. Drains were inserted in the lesser sac and pelvis, and a feeding jejunostomy was performed. The patient, however, continued to deteriorate postoperatively and succumbed to his illness 3 days after surgery
Further reading Click the link Acute pancreatits
Click here to Join the mailing list of HEALTHGUIDE
Join the mailing list!
Get the latest articles delivered right to your inbox!




